What is Homocysteine and Why Should You Care?
Most people have never heard of homocysteine, yet it quietly influences some of the most critical aspects of your health. If your doctor has flagged it on a blood test, or if you simply want to stay ahead of potential problems, understanding this marker could be one of the most useful things you do for your body this year.
Homocysteine is a naturally occurring amino acid, created when your body breaks down another amino acid called methionine. While it plays a role in metabolism, too much of it in the blood, a condition called hyperhomocysteinemia, is linked to a higher risk of heart disease, stroke, and other serious health issues.
For most people, this level stay in check through a balanced diet rich in B vitamins, specifically B6, B12, and folate. These nutrients help convert homocysteine into other beneficial substances. However, genetics, diet, and lifestyle can all cause levels to rise, and when they do, the health risks rise with them.
Why High Homocysteine Levels (Hyperhomocysteinemia) Matter
Doctors treat hyperhomocysteinemia as a biomarker, an indicator of potential health problems rather than a direct cause of disease. Think of it as an early warning signal. When levels climb too high, research has linked hyperhomocysteinemia to a range of serious conditions:
- Heart disease: Homocysteine may damage blood vessels, making it easier for cholesterol and plaque to build up, increasing the risk of heart attacks and strokes.
- Cognitive decline: Some studies suggest hyperhomocysteinemia levels might be linked to dementia and Alzheimer’s disease.
- Pregnancy complications: Hyperhomocysteinemia is associated with miscarriage, preeclampsia, and premature birth.
- Osteoporosis: High levels may weaken bones and increase the risk of fractures.
Who is at Risk for Hyperhomocysteinemia Levels?
Anyone can develop hyperhomocysteinemia, but certain groups carry a higher risk. Knowing whether you fall into one of these categories is the first step toward doing something about it.
- Older adults: As we age, our ability to absorb B vitamins declines, contributing to hyperhomocysteinemia.
- People with a poor diet: Those who consume low amounts of leafy greens, whole grains, and protein sources rich in B vitamins.
- Smokers and heavy drinkers: Both habits deplete vitamin B levels, contributing to hyperhomocysteinemia.
- Individuals with genetic mutations (MTHFR gene): Some people have a genetic predisposition that affects homocysteine metabolism.
- People with kidney disease: The kidneys help filter this metabolite, and impaired kidney function can lead to its buildup.
- Pregnant women: Adequate folate is crucial during pregnancy to prevent birth defects, and hyperhomocysteinemia can lead to complications.
Symptoms of Hyperhomocysteinemia Levels

Symptoms of Underlying Vitamin Deficiencies
In many cases, high homocysteine is caused by a lack of Vitamin B12, Vitamin B6, or Folate (B9). If these deficiencies are present, you might experience:
- Extreme Fatigue: Feeling constant exhaustion or lethargy regardless of rest.
- Neurological Sensitivities: Tingling, numbness, or a "pins and needles" sensation in the hands, arms, legs, or feet (paresthesia).
- Physical Weakness: A general lack of muscle strength or feeling "wobbly."
- Mouth Sores: Development of canker sores or a sore, reddened tongue (glossitis).
- Skin Changes: Paleness or a slight yellowish tint to the skin (jaundice).
- Mood Changes: Increased irritability or bouts of low mood.
Cardiovascular and Circulatory Warning Signs
High levels of homocysteine can damage the lining of the arteries and promote blood clots. While the damage happens internally, it can manifest as:
- Chest Pain (Angina): Discomfort or pressure in the chest, often during physical exertion.
- Shortness of Breath: Difficulty catching your breath, which may indicate heart strain.
- Circulatory Pain: Pain, swelling, or redness in the legs, which could be a sign of Deep Vein Thrombosis (DVT).
- F.A.S.T. Signs: Symptoms of a mini-stroke (TIA) or stroke, including facial drooping, arm weakness, or speech difficulty
Cognitive and Neurological Impacts
Sustained hyperhomocysteinemia is linked to neurological decline. Symptoms in this category often develop more gradually:
- "Brain Fog": Difficulty concentrating or a feeling of mental cloudiness.
- Memory Issues: Frequent forgetfulness or trouble recalling recent events.
- Confusion: Feeling disoriented or struggling with complex tasks that were previously easy.
- Dementia Progression: In older adults, high homocysteine is often associated with an increased risk of Alzheimer’s and other forms of cognitive decline.
Other Potential Indicators
- Slow Wound Healing: High homocysteine can interfere with the body's ability to repair tissues effectively.
- Digestive Issues: Chronic B-vitamin deficiencies can sometimes lead to nausea, diarrhea, or loss of appetite.
Because hyperhomocysteinemia is frequently asymptomatic until a major health event occurs, it is usually detected through a specific homocysteine blood test rather than through physical symptoms alone. If you suspect a vitamin deficiency or have a family history of early heart disease, consulting a professional for blood work is the standard diagnostic route.
Testing for Homocysteine Levels
A simple blood test can measure your homocysteine levels. Normal levels are usually below 15 micromoles per liter (µmol/L).
- Moderate: 15-30 µmol/L
- Intermediate: 30-100 µmol/L
- Severe: Over 100 µmol/L
What Can You Do to Lower Homocysteine Levels?
Here is the genuinely encouraging part. Hyperhomocysteinemia levels can often be managed through targeted diet and lifestyle changes. You have real, practical options.
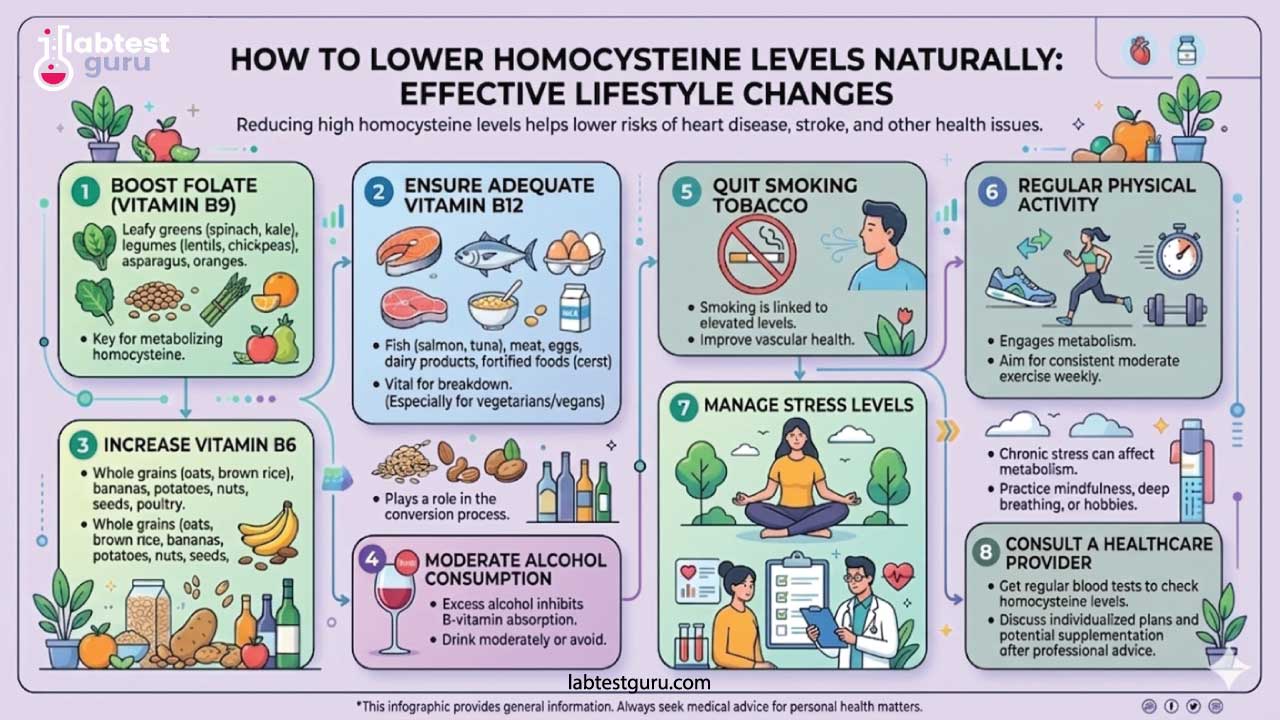
1. Boost Your B Vitamins
Since B vitamins are the key drivers of the breakdown of this metabolite, increasing your intake is the most direct lever you can pull. Focus on these three:
- Folate (Vitamin B9): Found in leafy greens, citrus fruits, beans, and fortified grains.
- Vitamin B6: Found in poultry, fish, bananas, and potatoes.
- Vitamin B12: Found in animal products like meat, eggs, dairy, and fortified plant-based foods.
For those with deficiencies or a genetic predisposition like the MTHFR mutation, B-vitamin supplements can be an effective and straightforward way to keep levels in check. Talk to your doctor before starting any supplementation.
2. Quit Smoking and Reduce Alcohol Consumption
Both smoking and excessive alcohol intake interfere with vitamin absorption and disrupt metabolism of the metabolite. Cutting back delivers benefits that extend well beyond this single marker, but your levels will likely be one of the first things to improve.
3. Eat a Balanced Diet
A whole-food diet rich in vegetables, fruits, whole grains, nuts, and seeds gives your body the raw materials it needs to process this metabolite efficiently. Simple, consistent eating habits tend to move the needle more than any single superfood.
4. Exercise Regularly
Physical activity supports a healthy heart and may also help keep the metabolite levels in check. You do not need an extreme programme. Regular, consistent movement is what counts.
5. Manage Underlying Health Conditions
Kidney disease and thyroid disorders can both contribute to hyperhomocysteinemia, so working with your healthcare provider to manage these conditions is an important part of the picture. Certain medications, including some used for epilepsy or chemotherapy, can also raise homocysteine levels. If you take any of these, ask your doctor whether monitoring your levels makes sense.
Complications of Untreated Hyperhomocysteinemia
If left unchecked, hyperhomocysteinemia can contribute to serious long-term conditions. This is not meant to alarm you. It is meant to make the case for acting early, while the changes required are still manageable.
- Cardiovascular disease: Increased risk of heart attack, stroke, and blood clots.
- Neurological disorders: Possible connections to cognitive decline, dementia, and even Parkinson’s disease.
- Pregnancy risks: Increased risk of miscarriage, neural tube defects, and preeclampsia.
- Bone health issues: Higher chances of osteoporosis and fractures.
The Bottom Line: Take Control of Your Health
Homocysteine is not a household name, but it is a meaningful indicator of how well your heart, brain, and overall metabolism are functioning. The fact that you can influence it through diet, lifestyle, and targeted supplementation puts genuine control in your hands.
If you fall into an at-risk group, or if any of the symptoms in this article resonated with you, ask your doctor to add this test to your next blood panel. A few informed changes today can make a measurable difference to your health in the years ahead.
Frequently Asked Questions (FAQs)
What causes high homocysteine levels?
The most common causes include:
- Vitamin Deficiencies: Insufficient intake or absorption of Vitamin B12, Vitamin B6, or Folate (B9).
- Genetics: Mutations in genes such as MTHFR (methylenetetrahydrofolate reductase) or CBS (cystathionine beta-synthase) can impair the body's ability to process homocysteine.
- Lifestyle Factors: Smoking and excessive alcohol consumption.
- Medical Conditions: Chronic kidney disease (which reduces homocysteine excretion), hypothyroidism, and certain types of anemia.
- Medications: Drugs like methotrexate, phenytoin, and carbamazepine can interfere with vitamin metabolism.
How is a homocysteine test performed?
It is a simple blood test, usually performed after a fast of 8 to 12 hours to ensure accuracy. Because homocysteine is unstable in blood samples, the plasma must be separated from the red blood cells quickly after collection to prevent false elevations.
Can high homocysteine be treated?
Yes. Treatment typically focuses on addressing the underlying cause. This often involves:
- Supplementation: Increasing intake of Folate, B12, and B6.
- Dietary Changes: Consuming more fruits, leafy green vegetables, and fortified grains.
- Management of Co-morbidities: Treating underlying kidney or thyroid issues.
Does lowering homocysteine always prevent heart disease?
While there is a clear correlation between high homocysteine and vascular risk, clinical trials have shown mixed results regarding whether vitamin supplementation significantly reduces the incidence of heart attacks in all populations. However, it remains a critical marker for diagnosing vitamin deficiencies and managing specific genetic conditions like homocystinuria.
Who should be tested for homocysteine?
Testing is generally recommended for individuals with:
- Unexplained blood clots or early-onset cardiovascular disease.
- Symptoms of B12 or folate deficiency (e.g., fatigue, numbness, or megaloblastic anemia).
- A family history of homocystinuria.
- Malnutrition or malabsorption syndromes.
Disclaimer: This information is for general knowledge and informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health.
References
- Hermann A, Sitdikova G. Homocysteine: Biochemistry, Molecular Biology and Role in Disease. Biomolecules. 2021 May 15;11(5):737. doi: 10.3390/biom11050737. PMID: 34063494; PMCID: PMC8156138.
- Finkelstein JD, Martin JJ. Homocysteine. Int J Biochem Cell Biol. 2000 Apr;32(4):385-9. doi: 10.1016/s1357-2725(99)00138-7. PMID: 10762063.
- Wijekoon EP, Brosnan ME, Brosnan JT. Homocysteine metabolism in diabetes. Biochem Soc Trans. 2007 Nov;35(Pt 5):1175-9. doi: 10.1042/BST0351175. PMID: 17956306.
- Bleich S, Hillemacher T. Homocysteine, alcoholism and its molecular networks. Pharmacopsychiatry. 2009 May;42 Suppl 1:S102-9. doi: 10.1055/s-0029-1214396. Epub 2009 May 11. PMID: 19434547.
- Temple ME, Luzier AB, Kazierad DJ. Homocysteine as a risk factor for atherosclerosis. Ann Pharmacother. 2000 Jan;34(1):57-65. doi: 10.1345/aph.18457. PMID: 10669187.
- Ferechide D, Radulescu D. Hyperhomocysteinemia in renal diseases. J Med Life. 2009 Jan-Mar;2(1):53-9. PMID: 20108491; PMCID: PMC5051482.
- Pizzorno J. (2014). Homocysteine: Friend or Foe?. Integrative medicine (Encinitas, Calif.), 13(4), 8–14.
- Son P, Lewis L. Hyperhomocysteinemia. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK554408/

