Decoding the 14 Markers: What Your Blood is Telling You
The comprehensive metabolic panel or also known as CMP is one of the most common tests your doctor will ever order, and it deserves more than a confused glance before you close the patient portal.
This single blood draw functions as a foundational diagnostic tool, giving us an accurate snapshot of your body's chemical balance and metabolism. When a doctor orders it, they want a broad overview of how your major organs are functioning. A comprehensive metabolic panel (CMP) measures 14 different substances in your blood, including proteins and electrolytes, making comprehensive metabolic panel (CMP) a routine test that can give your healthcare provider a picture of your overall physical health (1).
Liver Enzymes, Kidney Markers, and Electrolyte Balance
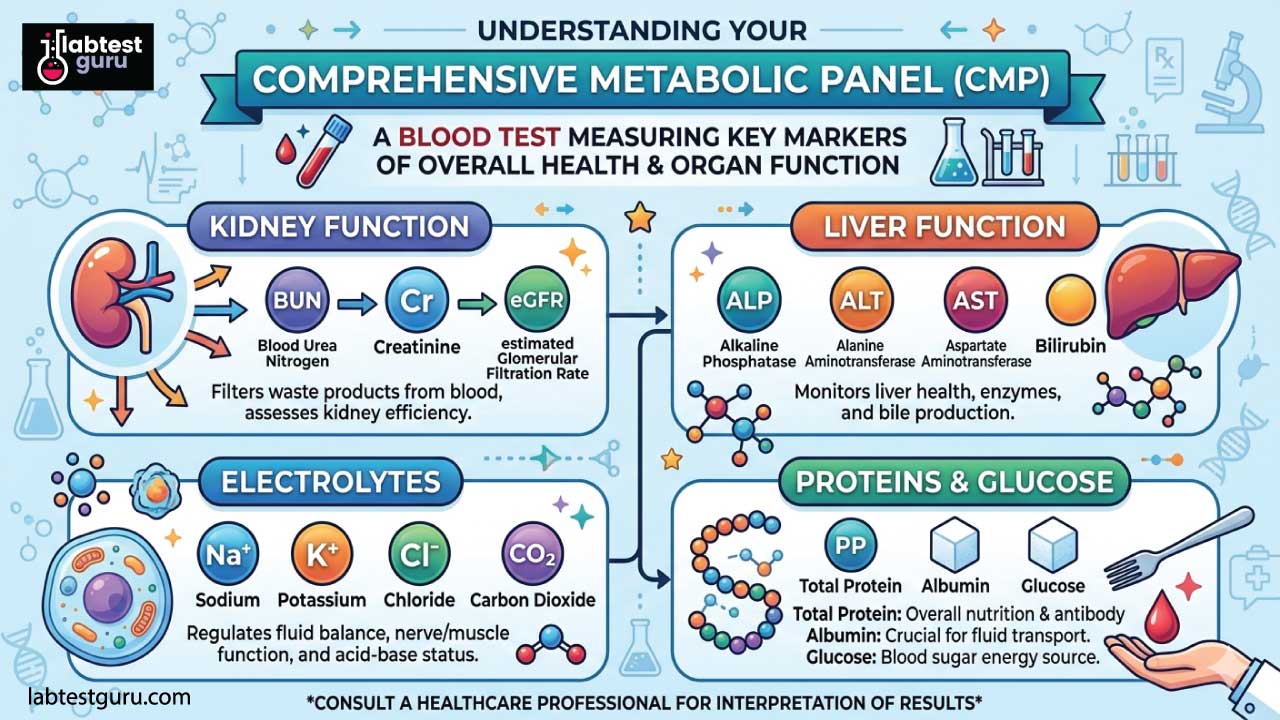
Pathologists group the 14 markers of comprehensive metabolic panel (CMP) into four distinct categories. First comes blood glucose, your body's primary energy source and a key early indicator for diabetes risk. Second is calcium, the mineral your bones, muscles, and nervous system all depend on to function properly.
Third, we look at your kidneys. Blood Urea Nitrogen (BUN) and creatinine are waste products your kidneys should be actively filtering from your blood, so elevated levels tell us something is worth investigating. Finally, we assess liver function and proteins: albumin, total protein, and liver enzymes including Alkaline Phosphatase (ALP), Alanine Aminotransferase (ALT), Aspartate Aminotransferase (AST), and bilirubin.
Blood Sugar
| Marker | What It Measures | Clinical Significance |
| Glucose | The primary sugar used by the body's cells for energy. | High: Diabetes, insulin resistance, or acute stress. Low: Hypoglycemia, excessive insulin, or poor nutrition. |
Kidney Function
| Marker | What It Measures | Clinical Significance |
| Blood Urea Nitrogen (BUN) | A waste product formed in the liver from protein breakdown and filtered by the kidneys. | High: Kidney impairment, severe dehydration, or heart failure. Low: Severe liver disease or malnutrition. |
| Creatinine | A waste product generated from normal, daily muscle breakdown and filtered by the kidneys. | High: Acute or chronic kidney disease, or severe muscle damage. Low: Low muscle mass or severe malnutrition. |
Electrolytes and Fluid Balance
| Marker | What It Measures | Clinical Significance |
| Sodium (Na) | An electrolyte vital for nerve signaling, muscle function, and maintaining blood volume and fluid balance. | High: Dehydration or specific kidney dysfunctions. Low: Fluid overload, heart failure, or medication side effects. |
| Potassium (K) | An electrolyte critical for maintaining normal heart rhythms, muscle contractions, and nerve impulses. | High: Kidney failure, cell damage, or medication side effects. Low: Diuretic use, vomiting, or diarrhea. |
| Chloride (Cl) | Works alongside sodium to regulate bodily fluids and maintain acid-base (pH) balance. | High: Dehydration or metabolic acidosis. Low: Heart failure, chronic lung disease, or prolonged vomiting. |
| Carbon Dioxide (CO2) | Reflects the amount of bicarbonate in the blood; crucial for maintaining the body's acid-base balance. | High: Severe respiratory issues or metabolic alkalosis. Low: Kidney disease, uncontrolled diabetes, or metabolic acidosis. |
| Calcium (Ca) | Essential for bone health, muscle contraction, blood clotting, and nerve signaling. | High: Hyperparathyroidism, certain cancers, or excess vitamin D. Low: Vitamin D deficiency, kidney disease, or hypoparathyroidism. |
Liver Function and Proteins
| Marker | What It Measures | Clinical Significance |
| Total Protein | The total amount of albumin and globulin proteins circulating in the blood. | High: Chronic inflammation, chronic infections, or multiple myeloma. Low: Liver disease, kidney disease, or severe malnutrition. |
| Albumin | A specific protein produced by the liver that transports nutrients and keeps fluid from leaking out of blood vessels. | High: Dehydration. Low: Liver disease, kidney disease (nephrotic syndrome), or systemic inflammation. |
| Alkaline Phosphatase (ALP) | An enzyme found primarily in the liver, biliary tract, and bones. | High: Bile duct obstruction, liver disease, or bone disorders (e.g., Paget's disease). Low: Zinc deficiency or malnutrition. |
| Alanine Aminotransferase (ALT) | An enzyme concentrated in the liver; it is released into the bloodstream when liver cells are damaged. | High: Hepatitis, fatty liver disease, or toxic liver injury. Low: Generally not clinically significant. |
| Aspartate Aminotransferase (AST) | An enzyme found in the liver, heart, and skeletal muscles. | High: Liver damage, severe muscle injury, or recent heart attack. Low: Generally not clinically significant. |
| Bilirubin | A yellow waste product produced during the normal breakdown of red blood cells, processed and excreted by the liver. | High: Liver disease (cirrhosis, hepatitis), blocked bile ducts, or hemolytic anemia. Low: Generally not clinically significant. |
Comprehensive Metabolic Panel (CMP) Reference Ranges
A Comprehensive Metabolic Panel (CMP) measures 14 key blood markers, but reference ranges can vary slightly by lab, age, sex, and units used (e.g., mg/dL vs. mmol/L). Always consult your doctor for personalized interpretation, as these are general adult ranges compiled from standard sources like Testing.com, Cleveland Clinic, and WebMD (4,5,6).
Comprehensive Metabolic Panel (CMP) Parameters and Ranges
| Parameter | Typical Range (Adults) |
| Glucose | 70-99 mg/dL |
| Calcium | 8.5-10.2 mg/dL |
| Sodium | 136-145 mEq/L |
| Potassium | 3.5-5.0 mEq/L |
| CO₂ (Bicarbonate) | 23-29 mEq/L |
| Chloride | 96-106 mEq/L |
| BUN (Blood Urea Nitrogen) | 6-20 mg/dL |
| Creatinine | 0.5-1.1 mg/dL (women); 0.7-1.3 mg/dL (men) |
| Albumin | 3.4-5.4 g/dL |
| Total Protein | 6.0-8.3 g/dL |
| ALP (Alkaline Phosphatase) | 30-120 U/L (women); 20-130 U/L general |
| ALT (Alanine Aminotransferase) | 4-36 U/L (women); 10-40 U/L general |
| AST (Aspartate Aminotransferase) | 8-33 U/L (women); 10-40 U/L general |
| Bilirubin (Total) | 0.3-1.9 mg/dL |
CMP vs. BMP: Which Test Do You Actually Need?
You may occasionally see a Basic Metabolic Panel (BMP) ordered instead of a comprehensive metabolic panel (CMP). Knowing the difference means you can ask better questions at your next check-up. Think of the BMP as the scaled-down version.
It covers only 8 of the 14 tests: glucose, calcium, the standard electrolytes, and the kidney markers BUN and creatinine. The liver enzymes and protein measurements are left out entirely. If you are monitoring your overall wellness or starting a new medication, the full 14-marker panel gives us the more complete picture that pathology relies on. When in doubt, ask for the full panel.
How AI is Personalizing Metabolic Treatment Plans
In the pathology lab, AI algorithms are being integrated to enhance the accuracy of test results, identify patterns in metabolic disorders, and facilitate personalized treatment plans. That is a significant shift from simply flagging a number as high or low. These tools can track subtle biological trends in your results over time, helping your doctor spot potential problems long before you feel any physical symptoms.
Who is Most at Risk? Understanding Demographic Vulnerabilities in Metabolic Health
For women in their thirties and beyond, metabolic health deserves serious attention. Hormonal changes, chronic stress, and lifestyle factors can all shift your metabolic baseline without you realising it. Metabolic syndrome, a cluster of conditions that elevate your risk of heart disease, stroke, and type 2 diabetes, affected a staggering 34.2% of US adults between 2007 and 2012 (2).
The risk, however, is not shared equally. The age-adjusted prevalence of metabolic syndrome in US women sits at approximately 23%, but the demographic disparities are stark. African American women face a rate 57% higher than men in their demographic. Mexican American women face a rate 26% higher than men in theirs (3). These numbers are not just statistics. They are a clear signal that certain women need to advocate loudly for regular, consistent screening.
Preparation and Process: What to Expect and How to Ensure Accuracy
Getting accurate results starts before you even walk into the clinic. You will typically be asked to fast for 10 to 12 hours before your blood draw for comprehensive metabolic panel (CMP), meaning nothing but water. Eating beforehand can temporarily skew your glucose and electrolyte levels, which undermines the entire point of the test. Keep drinking plain water, though. Dehydration can artificially elevate your kidney markers and makes the blood draw considerably harder.
| Myth | Reality |
| You must avoid all daily medications before a blood test. | Always ask your doctor. Many prescriptions should be taken on schedule with a small sip of water, while others might need to be paused. |
| A painful blood draw means the results will be inaccurate | While pediatric clinics use special techniques to keep children calm during a draw, temporary discomfort or a difficult vein does not alter the chemical composition of your blood sample |
Interpreting the Numbers: When to Talk to Your Doctor
After the lab processes your sample, you will receive a comprehensive metabolic panel (CMP) report showing your personal values alongside a standard reference range. Normal fasting glucose typically falls between 70 and 99 mg/dL, while normal calcium ranges from 8.5 to 10.2 mg/dL.
Why a "Normal" Result Doesn't Always Mean Perfect Health
Reference ranges are statistical averages. A result that lands just inside the "normal" bracket might still be outside your personal baseline, particularly if your numbers have been shifting over time. This is why routine monitoring matters. For patients managing chronic illnesses or taking intense antiviral medications, comprehensive metabolic panel (CMP) is absolutely vital for detecting early liver damage or identifying low protein levels linked to malnutrition.
If you see a number flagged in red or marked "out of range," take a breath before you panic. Minor fluctuations happen, caused by hydration levels, a recent illness, or even a hard workout the day before. Treat your comprehensive metabolic panel (CMP) results as an informed starting point for a real conversation with your physician. Ask them how these numbers fit into your broader health story. That conversation is exactly what this test is designed to start.
Frequently Asked Questions (FAQs)
How long does it take to get comprehensive metabolic panel (CMP) results?
In most cases, comprehensive metabolic panel (CMP) results come back within 24 to 72 hours, depending on your clinic or lab provider. Many healthcare systems now upload comprehensive metabolic panel (CMP) results directly to a patient portal, so you may see your numbers before your doctor has had a chance to review them with you. If that happens, resist the urge to self-diagnose. Wait for the follow-up conversation.
Can I drink coffee before a comprehensive metabolic panel (CMP) blood test?
No. Coffee, even black coffee with nothing added, counts as breaking your fast. Caffeine affects your metabolism and can temporarily alter glucose and liver enzyme readings. Stick to plain water for the full 10 to 12 hours before your draw.
How often should women get a comprehensive metabolic panel (CMP) done?
For most healthy women in their thirties and forties, once a year as part of a routine physical is a reasonable baseline. If you are managing a chronic condition, taking long-term medication, or have a family history of metabolic disorders, your doctor may recommend testing more frequently. The key word is routine. A single result tells you very little. A pattern of results over years tells you a great deal.
What happens if my comprehensive metabolic panel (CMP) results are abnormal?
An out-of-range comprehensive metabolic panel (CMP) result on its own is rarely a final answer. Your doctor will likely look at your full clinical picture, consider factors like recent illness, medications, or dehydration, and may order a follow-up test to confirm whether the reading reflects a genuine issue or a temporary fluctuation. Abnormal does not automatically mean serious. It means the conversation needs to continue.
Is a comprehensive metabolic panel (CMP) the same as a full blood count?
No, and this is a common point of confusion. A full blood count, sometimes called a complete blood count or CBC, measures the cellular components of your blood: red blood cells, white blood cells, and platelets. The comprehensive metabolic panel (CMP) focuses on the chemical and metabolic side, covering organ function, electrolyte balance, and protein levels. The two tests look at entirely different things and are often ordered together for a more complete picture of your health.
Disclaimer: This information is for general knowledge and informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health.
References
- https://my.clevelandclinic.org/health/diagnostics/22056-comprehensive-metabolic-panel-cmp
- Moore JX, Chaudhary N, Akinyemiju T. Metabolic Syndrome Prevalence by Race/Ethnicity and Sex in the United States, National Health and Nutrition Examination Survey, 1988–2012. Prev Chronic Dis 2017;14:160287. DOI: http://dx.doi.org/10.5888/pcd14.160287
- Bentley-Lewis, R., Koruda, K., & Seely, E. W. (2007). The metabolic syndrome in women. Nature clinical practice. Endocrinology & metabolism, 3(10), 696–704. https://doi.org/10.1038/ncpendmet0616
- https://www.testing.com/tests/comprehensive-metabolic-panel-cmp/
- https://my.clevelandclinic.org/health/diagnostics/22058-comprehensive-metabolic-panel-cmp
- https://www.webmd.com/a-to-z-guides/comprehensive-metabolic-panel
- Saklayen M. G. (2018). The Global Epidemic of the Metabolic Syndrome. Current hypertension reports, 20(2), 12. https://doi.org/10.1007/s11906-018-0812-z
- Abohashem S, Hassan I, Wasfy JH, Taub PR. Trends and Prevalence of the Metabolic Syndrome Among US Adults. JAMA. 2026 Jan 20;335(3):274-277. doi: 10.1001/jama.2025.21712. PMID: 41379435; PMCID: PMC12699394.
- Swarup S, Ahmed I, Grigorova Y, et al. Metabolic Syndrome. [Updated 2024 Mar 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459248/

